Self-harm and addiction – what is the connection
While self-harm may seem odd to most people, the fact is that it is a coping mechanism that many people choose to use to deal with their issues. We all have our ways of dealing with numerous problems that life throws at us, after all. While self-harm is harmful enough on its own, it may get worse if it is also coupled with addiction issues. Self-harm and addiction usually go hand-in-hand, fueling each other and creating an even worse situation. Luckily, help is readily available. If you happen to be living in the Keystone State, the best way to deal with self-harm and addiction is to get treatment at one of the dual diagnosis treatment centers in Pennsylvania. But how exactly is self-harm defined, why do people resort to it, what are the signs of self-harm, and how is it connected to addiction?
Jump to Section
How is self-harm defined?
The most common definition of self-harm is that it involves any behavior where someone intentionally causes harm to themselves. This includes anything from simply scratching at your skin, overeating/undereating, banging your head against an object, re-opening old wounds, biting or burning your flesh, etc. Basically, if you are doing any intentional damage to your body, no matter how big or small, it is considered to be self-harm.
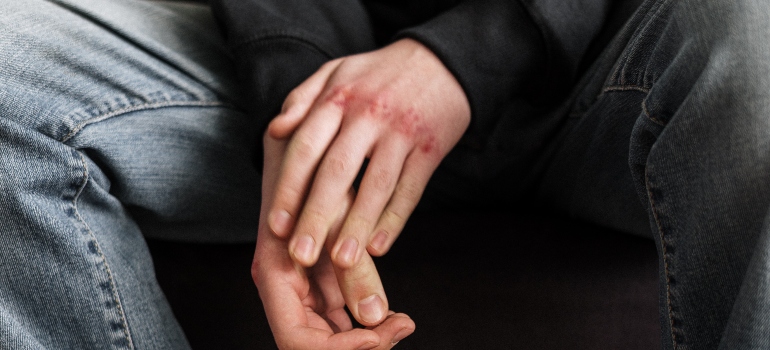
By itself, self-harm is considered to be a behavior and not a disorder. More commonly, however, self-harm is a symptom of an underlying mental health disorder or substance abuse. Therefore, the usual method of treating self-harm is to treat the underlying cause. For example, if addiction is the cause, you can enroll in a CBT treatment plan for substance abuse. If self-harm results from PTSD or a depression disorder, there are other treatments available.
Why do people self-harm?
Self-harm is a complex and multifaceted phenomenon, and its underlying causes can vary greatly from person to person. However, there are several common reasons why someone might engage in self-harming behaviors. One reason is to cope with overwhelming emotional pain or distress. People who self-harm may feel unable to express their feelings in words or may feel that others do not understand them. By inflicting physical pain upon themselves, they may find temporary relief from emotional pain. Furthermore, self-harm can be a form of self-punishment or self-purification. For example, you may feel guilty or ashamed of your thoughts, feelings, or actions and may believe that you deserve to be punished. By harming yourself, you may feel that you are paying for your perceived wrongdoings.
However, it is important to note that self-harm is not a solution to emotional pain or guilt. In fact, it can lead to further physical and emotional harm, perpetuating a cycle of self-destructive behavior. That being said, self-harm can also be a form of communication. Some people may feel that their emotional pain is not being recognized or validated by others and may resort to self-harm as a way of expressing their distress. By showing physical signs of their pain, they may hope to receive the support and understanding they need.
Gaining a sense of control
Additionally, some individuals may engage in self-harm as a way of gaining a sense of control or relief from anxiety. By focusing on the physical pain of self-harm, they may be able to temporarily escape from overwhelming feelings of anxiety or uncertainty. If this sounds similar to why some people abuse certain substances, it is because self-harm and addiction are quite similar in that regard. Luckily, treatments that work with addiction, such as DBT for substance abuse, will also work with self-harm. However, you might want to be careful when seeking treatment for self-harm only, as there might be underlying factors that need to be treated first.

Signs of self-harm
In some cases, it can be incredibly difficult to spot the signs of self-harm. This is due to the fact that people who engage in self-harm are usually very good at hiding their injuries. They are also quite adept at providing very convincing explanations. However, there are some signs that can show their true nature. Here are some of them you might want to be on the lookout for:
- Low self-esteem
- Sudden weight gain/loss
- Isolation
- Symptoms of depression
- Easily falling into tears
Of course, any signs of alcohol or drug abuse may indicate self-harm, as well. You may also notice unusual marks on the skin, random injuries, burns, cuts, etc. If you happen to notice any of the signs, it is usually best to act. While you might not want to jump to any conclusions, it is better to offer help without need than not to offer any help at all. Most of the time, however, if you think that someone is harming themselves, they are. Try to talk to the person and see what they have to say. Just remember that people who practice self-harm are very good at hiding it.
Can self-harm be addictive on its own?
While self-harm is inherently different than other harmful coping mechanisms (drugs, alcohol, etc.), it can still make you think that you can’t manage your life without it. There is ample evidence that self-harm can be addictive on its own, after all. In fact, one research study shows that more than 97% of people who practice self-harm also exhibit several addictive aspects as well. In other words, you can consider self-harm to be a behavioral addiction. Some of the most common aspects of behavioral addictions include:
- Noting a sense of relief during or after a particular behavior
- Seeing the behavior as the solution to their problems
- Continuing to exhibit the same behavior even though it causes distress
- Feeling a sense of tension before engaging in the behavior
Our brain chemistry may also contribute to the addictive nature of self-harm. Many medical experts believe that the brain activates our opioid and dopamine systems through self-harm. The opioid systems are responsible for lessening our stress and pain, while the dopamine systems involve learning and rewards. A person whose brain releases opioid and dopamine chemicals while engaging in self-harm will usually experience fast relief from intense emotions. As you might imagine, it is rather easy to get addicted to something like that.

How are self-harm and addiction connected?
There are several ways in which self-harm and addiction interact. First, substance abuse may actually be self-harm in certain situations. Most powerful substances, both illicit and legal, come with rather nasty side effects. A person may try to engage in self-harming behavior simply by abusing a certain substance.
However, most of the time, self-harm and addiction “fuel” each other. They coexist with one another and share many of the same risk factors. People who tend to engage in self-harming behavior usually do so because of extreme distress or emotional pain, much the same as those who turn to substance abuse. Over time, addiction and self-harm become intertwined, becoming almost impossible to set them apart.
The fact of the matter is that self-harm and addiction have similar causes. They can either be a form of escapism or a way to deal with difficult situations. Furthermore, both addiction and self-harm may be the result of an underlying mental health issue. On the bright side, that also means that anything that works on treating addiction may also work on self-harm. One of the most successful therapies that can deal with both self-harm and addiction is music therapy for substance abuse. This particular therapy tries to “resonate” and overtake the part of the brain that turns to self-harm and addiction to resolve its issues.
Addiction and self-harm are not always connected
While self-harm and addiction might be quite similar in most ways, they are not the same. In fact, most people who are addicted to a substance show no signs of self-harm behavior and vice versa. This serves to point out something that is very important: Addiction and self-harm are two distinct issues and each one needs to be treated on its own. However, the problem with self-harm and addiction is that the people who are suffering from them are not usually amenable to the prospect of treatment. Only a few decide to take a look at IOP in Pennsylvania, for example. The way in which most people decide to go to treatment is when someone else “forces” them to. To do that, however, the person who is forcing the treatment needs to understand the symptoms of addiction and self-harm first.
Symptoms of addiction and self-harm
The problem with recognizing the self-harm and/or addiction symptoms is that they may be unique to the individual. However, there are some common symptoms that may point that the person might be struggling with either.
The common symptoms of addiction may include:
- Being unable to control or reduce the use of alcohol or drugs
- Neglecting hobbies, relationships, and responsibilities
- Improved tolerance
- Spending a lot of time obtaining, using, or recovering from addictive substances
- Continuing to use drugs or alcohol despite negative consequences
You may also notice the following symptoms that may relate to self-harm:
- Wearing long sleeves on hot days
- Avoiding social interactions
- Unexplained bodily injuries (burns, cuts, bruises, etc.)
On their own, addiction symptoms might not indicate that an individual is engaging in self-harm. However, if you notice any of these symptoms alongside the previously mentioned symptoms of self-harm, it might indicate that the person is suffering from two ailments and not only one.
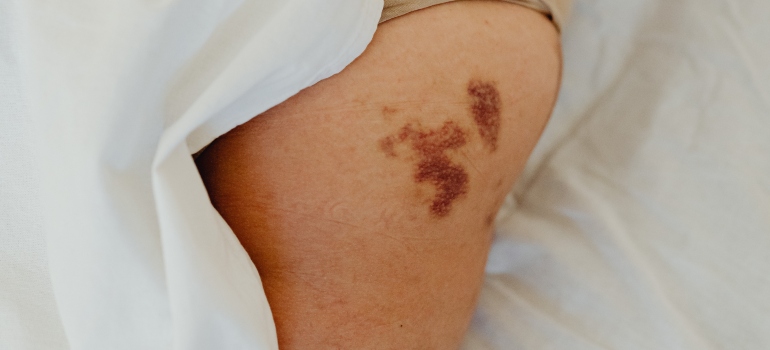
Regardless of the reason, spotting any of these signs may indicate that your loved one might have a problem with substance abuse, self-harm, or both. The best way to go about the situation is to try talking to your loved one first. Give them a chance to explain the situation and then verify their claims. If, after all that, you still believe that they have an addiction/self-harm problem, the best course of action is to seek treatment.
The best way to treat self-harm and addiction – Dual diagnosis treatment
Dual diagnosis treatment is an approach to treating individuals who have both a substance use disorder and a co-occurring mental health disorder. Also known as co-occurring disorders, these conditions often occur together, and each can exacerbate the symptoms of the other. Due to the fact that self-harm usually has deep roots in mental health disorders, dual diagnosis treatment is the perfect choice for someone that is struggling with self-harm and addiction.
Furthermore, dual diagnosis treatment is an integrated approach that recognizes the complex interplay between substance use and mental health disorders such as self-harm.
This treatment type offers the following:
- Comprehensive assessment
- Integrated treatment
- Medication management
- Psychotherapy
- Behavioral therapies
- Support groups

However, it is important to note that the treatment itself will vary based on individual needs. For example, no two patients receive the exact same treatment at Little Creek Recovery center. One person may benefit the most from CBT, for example, while another might require another behavioral therapy or even an entirely different approach. Self-harm and addiction are incredibly complicated issues that require a careful approach, after all. It is usually not enough to simply visit any residential treatment center Pennsylvania has to offer, you need to make sure that the treatment center has the knowledge and the ability to successfully perform dual diagnosis treatment. With this in mind, let’s take a look at what good dual diagnosis treatment looks like.
Comprehensive assessment
A comprehensive assessment is a critical component of dual diagnosis treatment, as it provides the foundation for developing a personalized treatment plan. The assessment process involves a thorough evaluation of your loved one’s physical, psychological, and social needs, as well as an assessment of their substance use and mental health disorders, including self-harm.
During the assessment process, your loved one may be asked to provide information about their medical history, substance use history, and mental health history. They may also undergo physical and psychological evaluations, such as blood tests, imaging studies, and psychiatric assessments. The assessment process may also involve interviews with family members, caregivers, and other healthcare professionals to obtain a more complete picture of the individual’s needs.
The goals of a comprehensive assessment in dual diagnosis treatment include:
- Identifying the presence and severity of substance use and mental health disorders
- Assessing the individual’s readiness for treatment
- Identifying any co-occurring medical conditions that may impact treatment
- Evaluating the individual’s social and environmental factors, such as family support, living situation, and employment status
- Identifying any barriers to treatment, such as financial or transportation issues
- Developing a personalized treatment plan that addresses the individual’s unique needs and circumstances

A comprehensive assessment is a critical first step in dual diagnosis treatment, as it provides the information necessary to develop a personalized treatment plan that addresses both substance use and mental health disorders such as self-harm. Without this assessment, every single one of Pennsylvania opioid treatment programs would be the same. Lastly, it is extremely important for your loved one to be honest and open during the assessment process, as this will help healthcare professionals to develop an effective treatment plan that meets their needs.
Integrated treatment
The integrated treatment approach in dual diagnosis recognizes that substance use and mental health disorders are often intertwined and can impact each other. For example, substance use may worsen the symptoms of self-harm, while untreated self-harm symptoms may increase the risk of substance use and addiction. Therefore, an integrated treatment approach that addresses both issues simultaneously is critical for successful recovery. However, integrated treatment does not mean that substance use and mental health disorders are treated in isolation, quite the opposite. The integrated treatment approach is actually a comprehensive and coordinated effort that addresses both issues in a holistic manner.
That being said, integrated treatment can be challenging, as it requires a high level of coordination and collaboration between healthcare professionals from different disciplines. It may involve a team of healthcare providers, including psychiatrists, addiction specialists, therapists, and social workers, working together to provide individualized care. This is why going to a specialized treatment center is usually the best idea. Treatment centers such as Little Creek Recovery have all the necessary medical professionals on staff, allowing us to offer this approach to our clients.
Lastly, integrated treatment recognizes the importance of addressing the social and environmental factors that may impact your loved one’s recovery. This may involve providing access to vocational counseling, family therapy, and other supportive services that can improve overall well-being and reduce the risk of relapse.
Medication management
Medication management is a very important component of dual diagnosis treatment. It can help to address both substance use disorder and co-occurring mental health disorders, such as self-harm. Dual diagnosis treatment can also use medications to reduce cravings for drugs or alcohol, manage withdrawal symptoms, and treat the symptoms of self-harm itself. However, medication management in dual diagnosis treatment can be quite complex. This is due to the fact that individuals with co-occurring disorders may require medications for multiple conditions. For example, if you are to undergo a heroin rehab in Pennsylvania while also having a self-harm diagnosis, it will take a team of experts to decide which medications are the best for your particular situation. This is why it is extremely important to choose your treatment center very carefully.
Psychotherapy
Almost every single addiction and/or self-harm treatment involves psychotherapy. Dual diagnosis treatment is no exception. One of the most important aspects of psychotherapy is that it allows for the creation of healthy coping mechanisms. Over time, psychotherapy removes the need to rely on self-harm to manage stress levels and introduces other coping skills.
Many people don’t understand the difference between psychotherapists and behavior therapists. While they might be similar, they are far from being the same. Psychotherapy involves talking to a mental health professional in order to better understand themselves. Throughout the course of the therapy, the patient will gain a better understanding of the issues they are facing and will learn how to handle them.
Behavioral therapies
Behavioral therapy aims to make direct connections between behaviors and solutions. This active approach to treatment is the reason why CBT (Cognitive Behavioral Therapy) and DBT (Dialectical Behavior Therapy), and MI (Motivational Interviewing) are dual diagnosis treatment staples. What behavioral therapies do is create concrete behavioral changes in their patients. This is what makes these therapies so powerful when it comes to dealing with both self-harm and addiction. Aside from CBT, DBT, and MI, there are many other behavioral therapies available, such as:
- Acceptance and commitment therapy (ACT)
- Problem-solving therapy
- Desensitization
- Compassion focused therapy
- Metacognitive therapy
- Cognitive analytic therapy
- Exposure and response prevention therapy
- Mindfulness-based cognitive therapy

Of course, the therapy type that will be used in dual diagnosis treatment will depend on the individual needs of the patient.
Support groups
Lastly, dual diagnosis treatment incorporates support groups. However, since people who engage in self-harm usually have a problem with social activities, this part of the treatment is slowly phased in. On the other hand, support groups are one of the best ways to manage addiction. There are three primary types of support groups:
- Peer support groups
- Support groups with friends and family members
- Online support groups
- Other support groups
While support groups may be useful during treatment, they are most useful after the treatment is over. Getting in touch with people who are struggling in a similar manner has all sorts of positive benefits. Relapse potential is lower, sharing life experiences can be extremely fun, and it is a very nice social activity on its own. Some people enjoy peer support groups the most while others may find themselves most comfortable in a friends&family support group.
Overall, the self-harm and addiction combination can be incredibly difficult to deal with, but not impossible. Treatment is readily available, all you need to do is reach out!