How Nurses and Doctors Provide Medical Detox Support
Begin TodayHow nurses and doctors provide medical detox support involves monitoring withdrawal symptoms, managing medications, ensuring patient safety, offering emotional care, and creating personalized treatment plans that help individuals detox safely and begin recovery under professional medical supervision.
Jump to Section
Detox can feel scary when you do not know what to expect, especially if withdrawal symptoms have already started. That is why it helps to know how nurses and doctors provide medical detox support in a safe, steady way. Doctors check your health, choose the right medications, and respond if symptoms become risky. Nurses stay close through the process, monitor vital signs, track changes, and help you feel as comfortable as possible. If you are looking for substance abuse treatment Pennsylvania rehab centers offer, medical detox can be the place where your body starts to stabilize and your next step in treatment becomes clearer.
Medical Detox Support From Nurses And Doctors
Detox starts with care that looks at your whole situation, not only the substance leaving your body. You may feel scared, sick, or unsure about what comes next. A trained team can help you stay safer while your body adjusts.

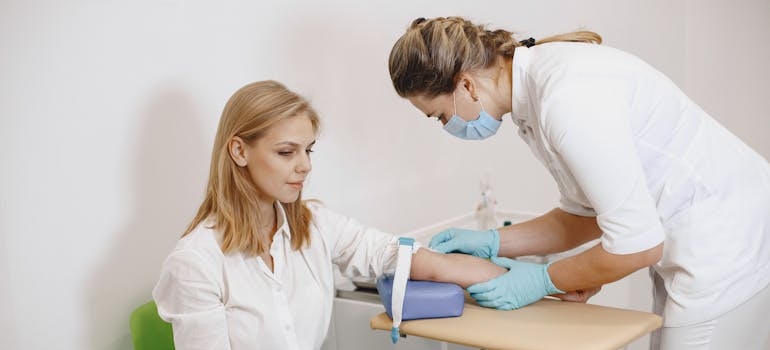
Initial Health Assessment
Before detox begins, the care team needs a clear picture of your health, substance use, symptoms, and risks. During the first assessment, the detox team usually checks several important areas before treatment begins, including:
- Review what substances you used, how much, and when you last used.
- Check blood pressure, pulse, breathing, temperature, pain, sleep, and hydration.
- Ask about seizures, severe withdrawal, overdose history, injuries, or health problems.
- Review mental health symptoms, panic, depression, trauma, and safety concerns.
- Look at prescriptions, allergies, and possible medication risks.
- Decide whether you need close monitoring, medication, fluids, or urgent medical help.
Withdrawal Risk Screening
Withdrawal can change fast, so risk screening helps your team act before symptoms become dangerous. Doctors and nurses look at your substance use, health history, and current symptoms to judge how closely you need to be watched. This is also when many people ask, when is it time to go to detox, especially if they feel shaky, sick, scared, or unable to stop safely.
A careful screen may show risks like seizures, dehydration, high blood pressure, confusion, or severe cravings. It can also reveal mental health concerns that need support during detox. This is how nurses and doctors provide medical detox support with safety in mind. Instead of waiting for a crisis, they use screening to plan care early, reduce fear, keep you stable, protect your health, and guide the next decision.
Medication Planning
Medication planning helps make detox safer and more manageable. Doctors choose medications based on what you are withdrawing from, your health, your symptoms, and your level of risk. Nurses then help give those medications, watch how you respond, and report changes quickly. This matters because the right medication can ease anxiety, nausea, sleep problems, pain, cravings, or dangerous withdrawal effects.
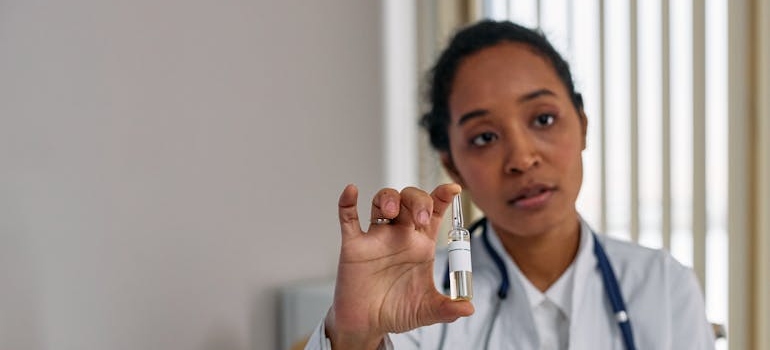
In some cases, ongoing care may include medication assisted treatment Pennsylvania options after detox, especially for opioid or alcohol use disorders. This plan should never feel random. Your team adjusts doses, watches side effects, and explains why each step matters. That is how nurses and doctors provide medical detox support in a way that treats comfort, safety, and your next steps with care each day.
How Doctors Manage Detox Safely
Doctors help keep detox from becoming a guessing game. They look at your symptoms, health risks, and past withdrawal history, then choose a plan that can change as your body changes. Their work is not only about medicine. It is also about timing, safety, and clear decisions.
Prescribing Withdrawal Medications
Withdrawal medications can reduce symptoms that feel hard to handle alone. In an adult inpatient medical detox setting, doctors may prescribe medicine for anxiety, nausea, sleep problems, cravings, high blood pressure, or seizure risk. The exact plan depends on the substance, your health, and how your symptoms change during care. A doctor may start with one dose, then raise or lower it after checking your response.
Nurses help by giving the medicine on time and reporting any side effects. This teamwork matters because withdrawal can shift quickly. You should not have to guess whether a symptom is normal or dangerous. A medical team watches those changes closely, so your care stays safer, more controlled, and focused on helping your body settle without extra harm today and move toward treatment safely.
Monitoring Medical Complications
Some withdrawal symptoms feel uncomfortable, while others can become serious without fast care. While detox is happening, doctors and nurses closely watch for serious symptoms and health concerns such as:
- High blood pressure, fast pulse, chest pain, fever, sweating, shaking, or breathing changes.
- Seizures, confusion, severe agitation, hallucinations, fainting, or loss of awareness.
- Dehydration, vomiting, diarrhea, poor food intake, weakness, or signs of low fluids.
- Worsening pain, infection concerns, injuries, or medical issues hidden by substance use.
- Severe anxiety, panic, depression, self-harm thoughts, or unsafe behavior.
- Medication side effects, allergic reactions, oversedation, or symptoms needing a dose change.
Adjusting Care Plans
Your detox plan should not stay the same if your symptoms change. Doctors review your progress and decide whether you need more monitoring, different medication, extra fluids, lab work, or another level of care. Nurses add important details because they see how you feel through the day and night. This is one reason tailored detox programs matter.
They give the team room to respond to your real needs instead of forcing one plan on every person. You may need more support on one day and less the next. That does not mean you are failing. It means your body is moving through withdrawal. Careful changes show how nurses and doctors provide medical detox support while lowering risk, improving comfort, and preparing you for rehab when detox is complete and you feel steadier.
What Detox Nurses Do During Treatment
Nurses are often the people you see the most during detox. They check on you, answer questions, notice changes, and help you through hard moments that can feel overwhelming. Their care is steady, practical, and personal at the same time. You may feel more comfortable speaking honestly with them as symptoms change.
Checking Vital Signs
Vital signs give the detox team important information about how your body is handling withdrawal. Nurses check blood pressure, pulse, breathing, temperature, oxygen levels, and pain throughout the day. These numbers may seem simple, but they can show when symptoms are becoming risky. A fast heart rate, rising blood pressure, or fever may point to serious withdrawal problems that need quick care.
Nurses also watch how you look, move, sleep, eat, and respond to medication. They report changes to doctors so treatment can adjust before symptoms get worse. This close attention helps people feel safer during detox because someone is always watching for signs of trouble. It also shows how nurses and doctors provide medical detox support through constant care, fast communication, and steady medical monitoring from the beginning of treatment until symptoms become more stable.
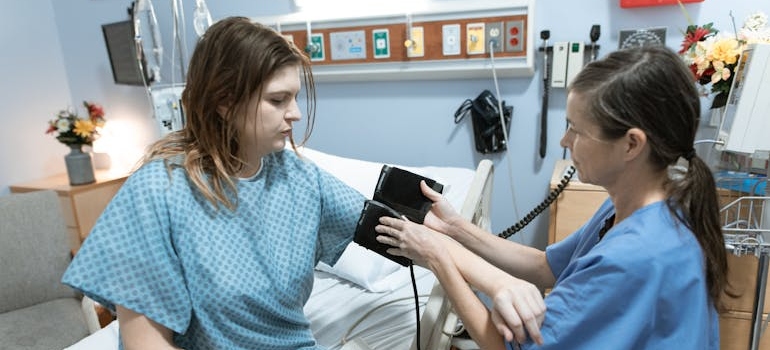
Tracking Withdrawal Symptoms
Withdrawal symptoms can change from hour to hour, which is why nurses track them closely during detox. They ask how you feel, check physical symptoms, and look for emotional or mental changes that may need attention. Symptoms may include shaking, sweating, nausea, anxiety, body pain, cravings, confusion, or trouble sleeping. Nurses record these changes so doctors can decide if treatment needs to shift. This kind of tracking is also important in Pennsylvania opioid treatment programs where withdrawal symptoms may continue even after the first days of detox.
Nurses help people stay honest about cravings and discomfort without feeling judged. That support matters because people often hide symptoms when they feel afraid or embarrassed. Careful symptom tracking shows how nurses and doctors provide medical detox support while helping patients stay safer, calmer, and more prepared for the next stage of recovery and treatment.
Providing Patient Comfort And Support
Detox can feel stressful, lonely, and physically draining, especially during the first days of withdrawal. To help patients feel safer and more comfortable during detox, nurses often provide support in ways like:
- Bring water, snacks, blankets, clean clothes, and comfort items when possible during care.
- Help patients rest by lowering noise, dimming lights, and creating a calmer room environment.
- Answer questions honestly so patients understand symptoms, medications, and what may happen next.
- Encourage hydration, nutrition, movement, hygiene, and healthier sleep habits during detox treatment.
- Support patients through fear, panic, cravings, emotional stress, or moments of frustration.
- Notice emotional changes and report serious concerns to doctors or mental health staff quickly.
Moving From Detox To Rehab
Detox can help your body stabilize, but recovery needs more support after withdrawal symptoms ease. This next step gives you space to work on triggers, habits, mental health, and daily structure. A good team should help you plan instead of leaving you unsure.

Creating A Next-Step Treatment Plan
A next-step treatment plan helps you know what happens after detox, before stress or cravings pull you back into old patterns. Your care team may talk with you about rehab, therapy, medication, family support, transportation, and safe housing. They may also review what type of program fits your needs. Some people need residential care, while others may move into outpatient treatment.
If opioids are involved, the plan may include support connected to heroin rehab centers or ongoing medication care. This plan should feel clear, not rushed. You deserve to know why each step is recommended and how it helps. Planning early can lower relapse risk because you leave detox with direction, support, and a treatment path that fits your health, your safety, and your real life needs.
Transitioning Into Residential Rehab
Moving into rehab after detox can feel like a big step, but it can also bring relief. Detox helps your body get through withdrawal, while rehab helps you work on the reasons substance use became part of your life. A residential drug and alcohol rehab center in Pennsylvania can give you daily structure, therapy, peer support, and space away from triggers.
This matters because early recovery often feels fragile. You may feel better after detox, but cravings, stress, and old habits can still return quickly. Rehab gives you more time to build skills, talk through hard issues, and learn how to handle life without substances. A smooth handoff from detox to rehab keeps you from feeling alone between levels of care and helps you stay connected to support.
Building Long-Term Recovery Support
Long-term recovery works better when you leave detox and rehab with real support around you. Before treatment ends, the recovery team may help patients build long-term support through services and planning such as:
- Set up therapy, medical appointments, support groups, or recovery meetings before discharge.
- Talk through triggers, cravings, stress, sleep, relationships, and unsafe places or people.
- Build a relapse prevention plan that feels clear, realistic, and easy to follow.
- Include family or trusted loved ones when support at home can help recovery.
- Plan for sober housing, work, transportation, medication care, and follow-up treatment needs.
- Keep treating mental health concerns that may affect substance use and relapse risk.

Start Recovery With Safe Medical Detox
Medical detox is not something you have to face alone. When withdrawal feels unsafe, painful, or hard to control, trained medical care can protect your health and give you steady support. Knowing how nurses and doctors provide medical detox support can help you see why this step matters. Doctors manage the medical side, while nurses stay close to your daily needs and watch for changes. Together, they help reduce risks, ease symptoms, and prepare you for the next stage of care. If you or someone you love needs help, reaching out for medical support can be the first clear step toward treatment, stability, and a better chance at lasting recovery.
Frequently Asked Questions
How do doctors detox patients?
Doctors detox patients by evaluating their physical and mental health, monitoring withdrawal symptoms, prescribing medications when needed, and creating personalized treatment plans to help patients safely manage substance withdrawal and begin recovery.
What is the role of a detox nurse?
A detox nurse monitors vital signs, administers medications, supports patient comfort, tracks withdrawal symptoms, and communicates with doctors to ensure patients receive safe and effective care throughout the detox process.
How do nurses treat alcohol withdrawal?
Nurses treat alcohol withdrawal by monitoring symptoms, checking vital signs regularly, administering prescribed medications, providing hydration and nutritional support, and helping patients stay stable and comfortable during detox.
Can medical detoxification be a medical necessity?
Yes, medical detoxification can be medically necessary for individuals experiencing severe withdrawal symptoms or health risks related to substance dependence, especially when withdrawal could lead to dangerous complications without professional supervision.













